Need a dermatologist for your skin problems?
Our team will create you a custom care plan
Our team are experts in everything skin and we can help you live a happier and more confident life through better skin health.
Learn more Make a bookingWe treat all skin conditions in our South Melbourne clinic with a broad range of therapies. Make an appointment today and we’ll find a skin care treatment plan that works for you.

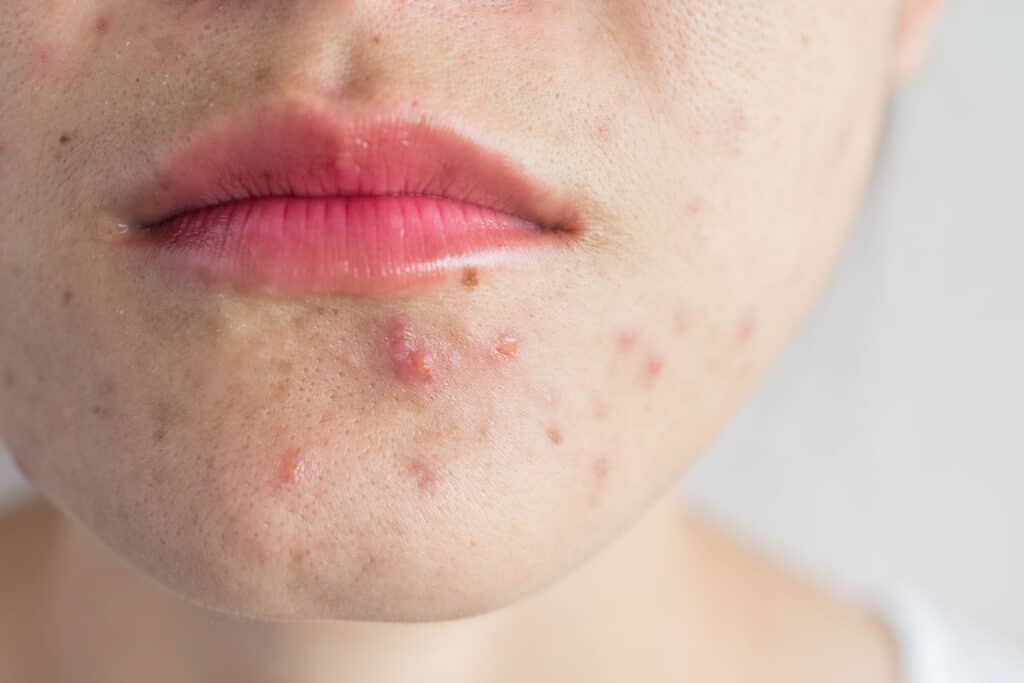
Acne is a potentially permanently scarring condition with most cases occurring during puberty, correlating with hormonal changes. Other medical conditions can also contribute to acne such as polycystic ovarian syndrome certain medical conditions.
It affects both teenagers and adults, caused by an overproduction of skin sebum (oil) from sebaceous glands, which then blocks pores, leading to pimples, blackheads, white-heads and nodular acne lesions.
In some cases, the severe acne lesions may lead to scarring [link to acne scarring in glossary] and hence it is important to gain control of acne quickly before this happens. We are proud to have the best acne dermatologists in Melbourne for your acne solutions.
Mild acne can be treated with over-the-counter products and topical agents. Some mild acne can even be treated with skin peels and cosmeceuticals which are available at our clinic.
More severe acne will need treatment with oral medications such as anti-inflammatory topical or oral antibiotics, topical vitamin A preparations, the oral contraceptive pill, anti-androgen tablets and isotretinoin (oral vitamin A tablets). In Australia isotretinoin prescriptions are restricted for dermatologists to prescribe only.
Our dermatologists will tailor an acne management plan for the best result.
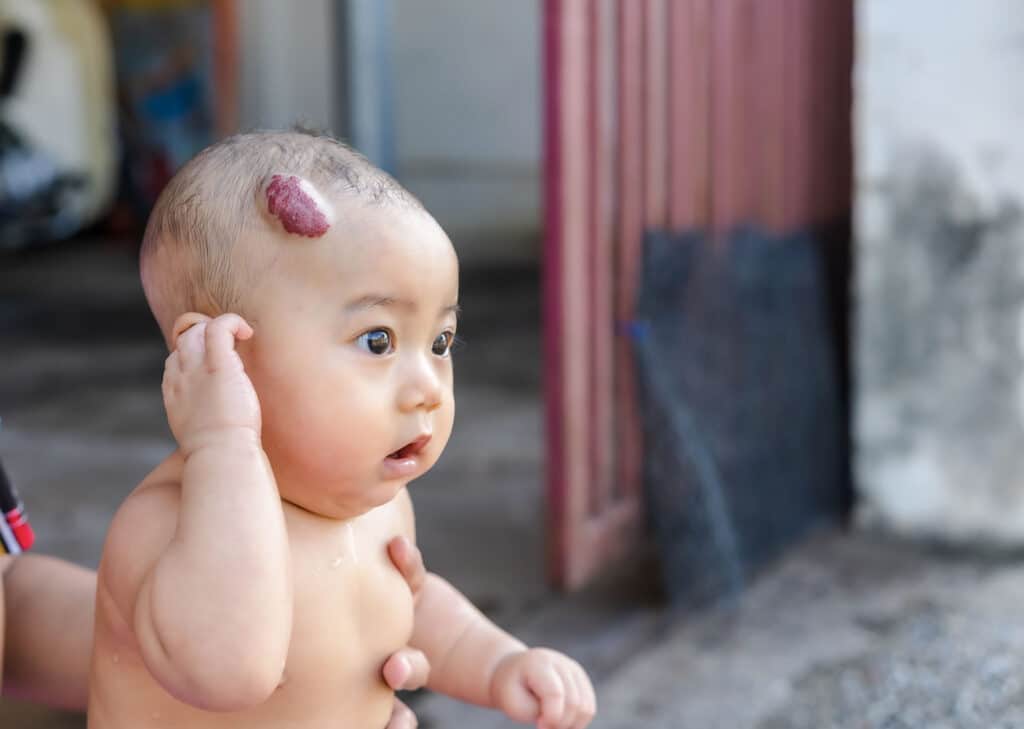
Birthmarks are marks on the skin that are present at birth. They can appear on any part of the body. Often, they are of no concern and they will fade over time. Some birthmarks warrant treatment for aesthetic reasons and others can lead to complications over time.
We use a range of treatments including corticosteroid injections, Interferon, laser therapy, and only if absolutely necessary, surgery.
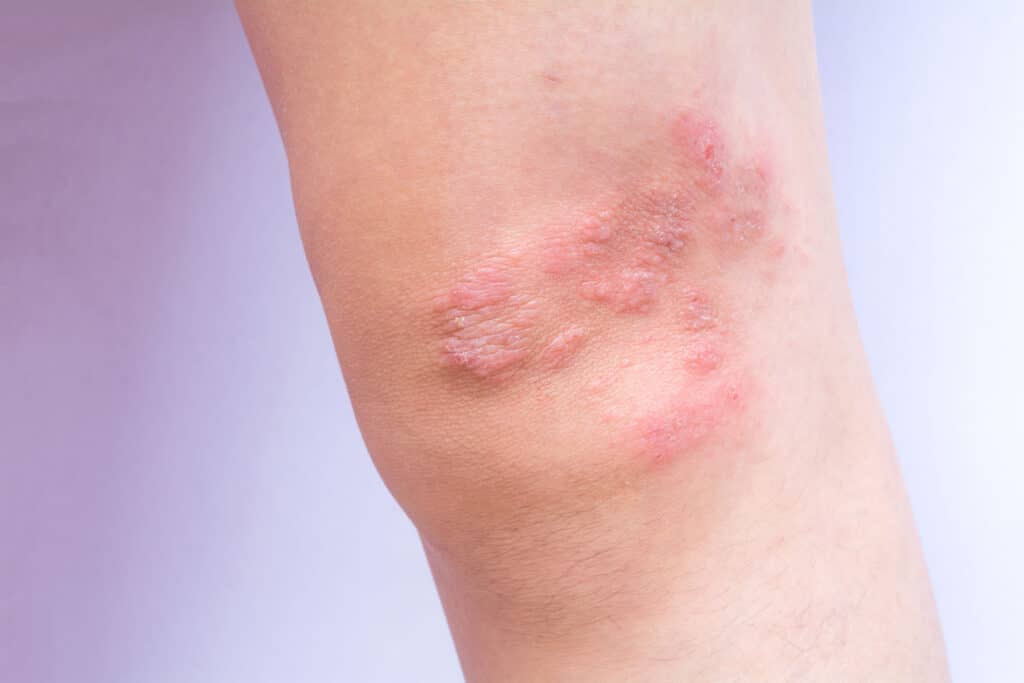
Eczema, or atopic dermatitis, is a common complaint in our patients, especially with Melbourne’s dry weather, and can affect people of all ages. It is a very common skin condition, affecting about 1 in every 5 people at some time in their lives.
Eczema results in dry, red, itchy skin, which may crack and bleed, and may be quite uncomfortable for patients. Eczema can also sometimes become secondarily infected.
There are multiple underlying factors contributing to eczema including hereditary and environmental factors. Triggers include environmental factors, such as dust mites, pollen, grasses, sweat, overheating, and many other substances. Eczema can also coincide with asthma and hayfever.
Research has shown that a genetic mutation of fillagrin, leading to poor skin barrier function is the key in the appearance of eczema. Treatment needs to be systematic and targeted and includes stopping excess soap use and changing to more moisturising products to restore the skin barrier.
Prescription treatment ranges from creams and tablets to settle down the inflammatory process to UV (light) phototherapy. Occasionally antibiotics may also be needed to treat any secondary infection. For more severe cases, oral immunosuppression may be required and this needs to be undertaken with an experienced dermatologist for the best outcome.
Wet dressings can also be helpful for eczema control. Check out our video on the technique of wet dressings for more information.
Dermatologists at Hope Dermatology are experts in eczema care plans for you and your family.
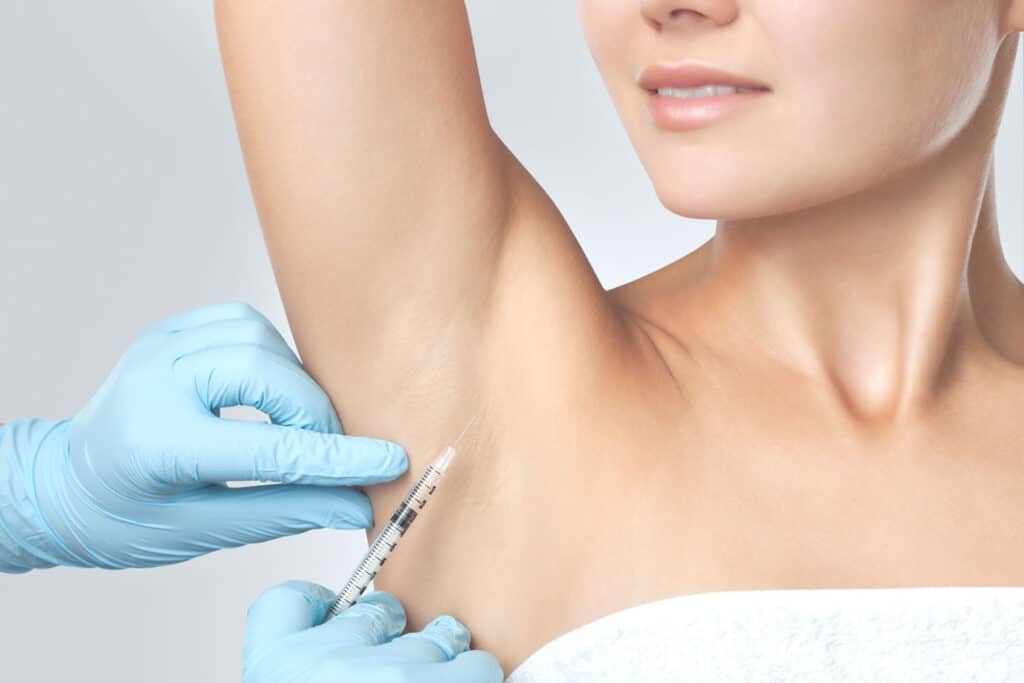
Hyperhidrosis is a condition characterised by excess sweating. It can be generalised or localised to certain body areas (for example, the underarms). Hyperhidrosis can be a sign of a different underlying conditions. Treatment can include topical creams, anti-sweating injections, iontophoresis bath treatments, laser and oral medication to reduce sweating.
For axillary (underarm) hyperhidrosis, dermatologists can offer injections directly into the underarm skin to reduce the sweating. There is a Medicare Rebate for this procedure and these injections can be performed every 4 months to control the sweating. Please contact us or book online for an appointment.
Genital skin problems can be common and often cause distress, embarrassment and be painful or itchy, interfering with relationships, self-image and sexual functioning. Some genital disorders are contagious, including sexually transmitted diseases however there can be many other causes. Diagnosis is made via detailed patient history and skin examination and may include blood tests, skin biopsy or swabs from the affected area.

There are a number of conditions that can cause hair loss. Causes can be multifactorial and include hereditary, autoimmune, non-scarring or scarring and stress response. Conditions we commonly see in terms of hair loss include the following: telogen effluvium (“shedding response hair loss”), androgenetic alopecia (female pattern and male pattern baldness), alopecia areata (autoimmune hair loss), scarring hair loss (discoid lupus erythematosus, lichen planopilaris, folliculitis decalvans).
The distinction between scarring and non-scarring hair loss is important as there is potential for regrowth with the non-scarring conditions. With the scarring conditions, the aim of treatment is to prevent the condition from worsening; but unfortunately with scarring hair loss, once the hair is gone it is gone forever. Occasionally in the same patient there can be both non-scarring and scarring processes happening.
Our dermatologists will assess your hair loss thoroughly and this will include taking a full personal and family history, medication history and examination. Depending on the type of hair loss, blood tests and a scalp biopsy may be relevant to determine the type of hair loss you are suffering from. Treatments for hair loss do depend on the underlying condition causing your hair loss and this will be explained to you in the detailed consultation.
Treatments including topicals, tablets and also cosmetic camouflage techniques.
Our dermatologists are expertly trained in the early diagnosis and treatment of hair loss conditions. Dr Hope Dinh has published extensively on hair loss conditions and this is her area of sub-specialisation and interest.

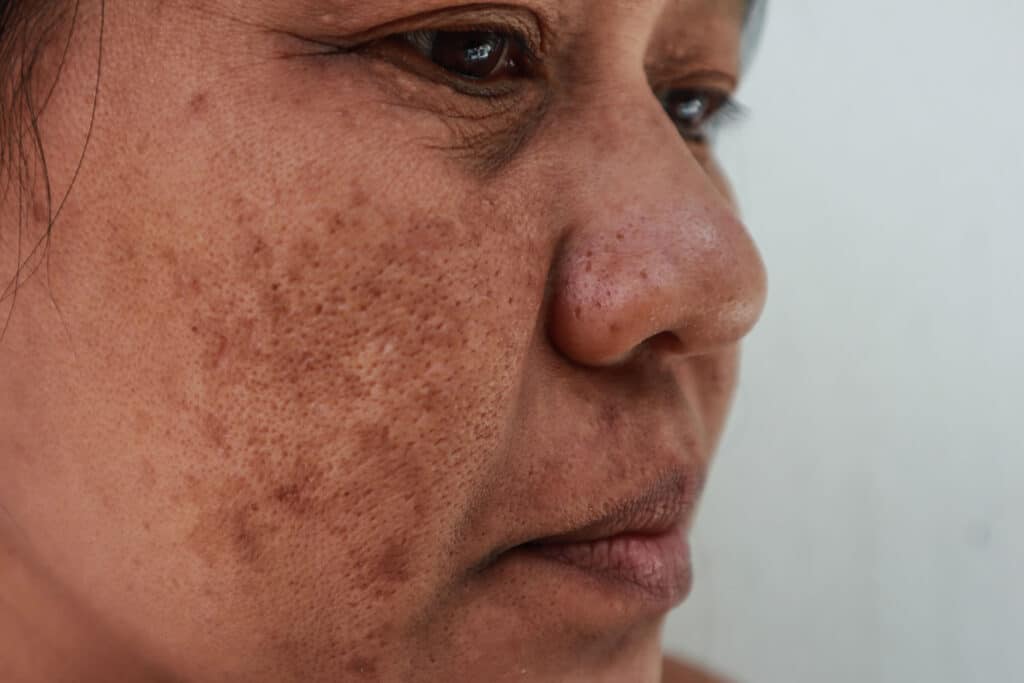
Melasma (or chloasma) is a common skin disorder, which presents with darkening of the facial skin, usually on the cheeks, forehead and around the mouth.
It is a symmetrical, blotchy, darkening of the skin that is chronic and can be distressing for sufferers. It commonly affects women more so than men, manifesting around the ages of 20-40. It results from an overstimulation of melanin by melanocytes, the pigment producing cells.
Multiple contributing factors are thought to be at play including genetics, darker skin type, ultraviolet exposure and hormones (from pregnancy and hormonal contraceptives), other medications and inflammation from cosmetics such as perfumes or soaps.
Treatment options include topical bleaching creams, strict sun protection with SPF 50+ broad spectrum sunscreen and cessation of contributing hormonal contraceptives. Recently, oral tranexamic acid tablets have been successful in reducing pigmentation. Peels and laser can also be cautiously used.
Speak to our dermatologists and cosmetic nursing team about the most suitable options for your skin.
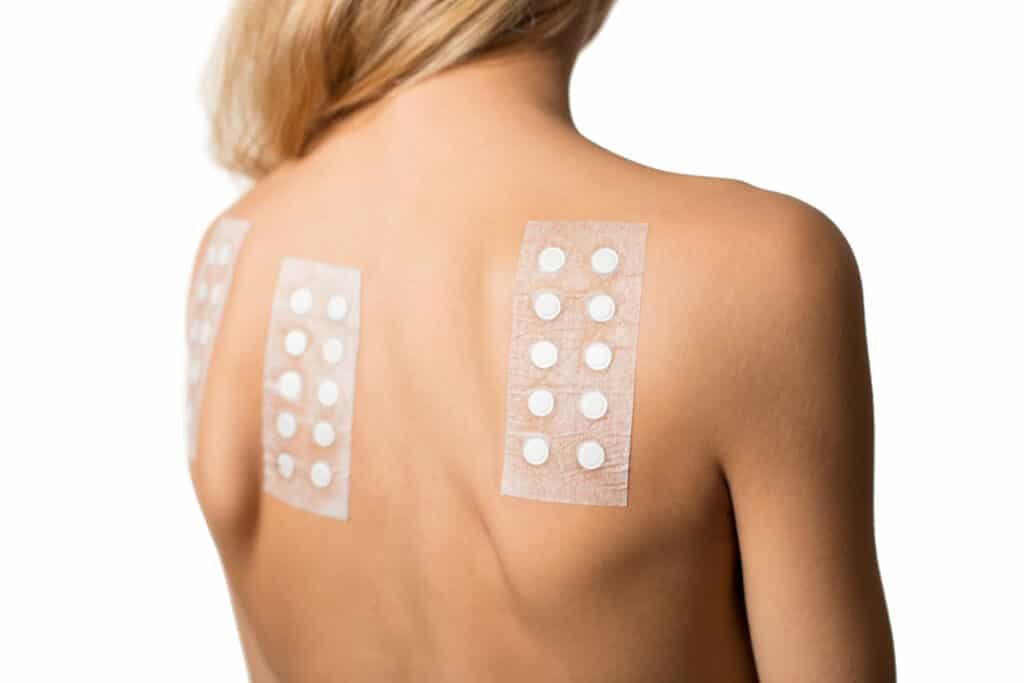
Patch testing is a procedure used to identify the cause of allergic contact dermatitis. Small patches are applied to the back and no needles are required.
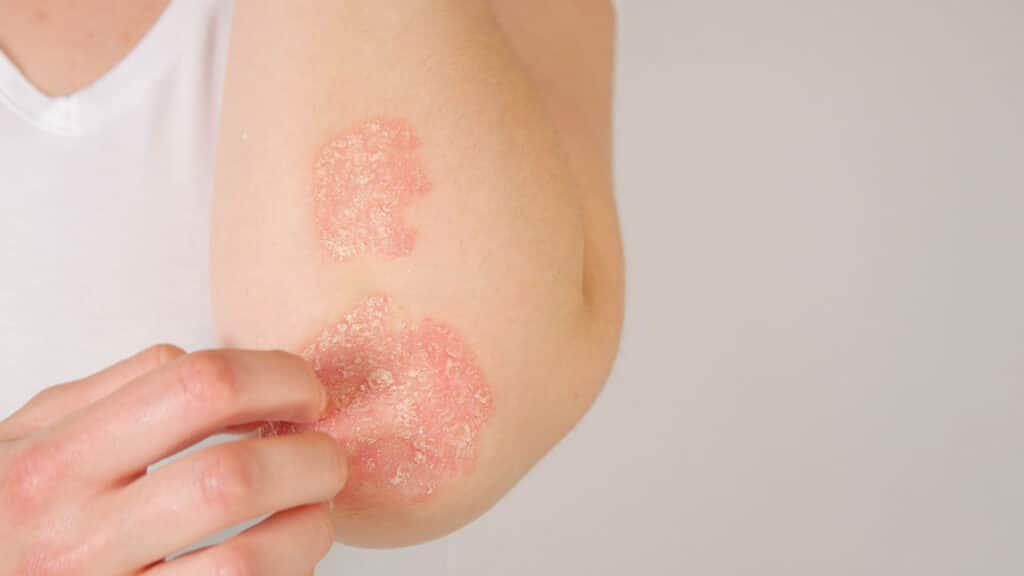
Psoriasis can be very cosmetically distressing for our patients. Recent research has revealed that in patients with psoriasis, the inflammatory process may not just be localised to the skin and hence it is even more important to diagnose and treat this condition promptly.
This is a chronic, genetic condition that causes well-defined large red, scaly plaques to appear on the skin. These red areas have a silvery superficial appearance and develop on the elbows, knees, scalp and chest. The nails and joints can also be involved.
Treatment options include creams, ultraviolet phototherapy, and a few different types of tablets (such as methotrexate, cyclosporin or acitretin). More recently, injections of Biologics are available and highly effective. In Australia, only Dermatologists can prescribe PBS (Pharmaceutical Benefits Scheme)-funded Biologics for skin psoriasis. Our dermatologists are experts in psoriasis diagnosis and management.
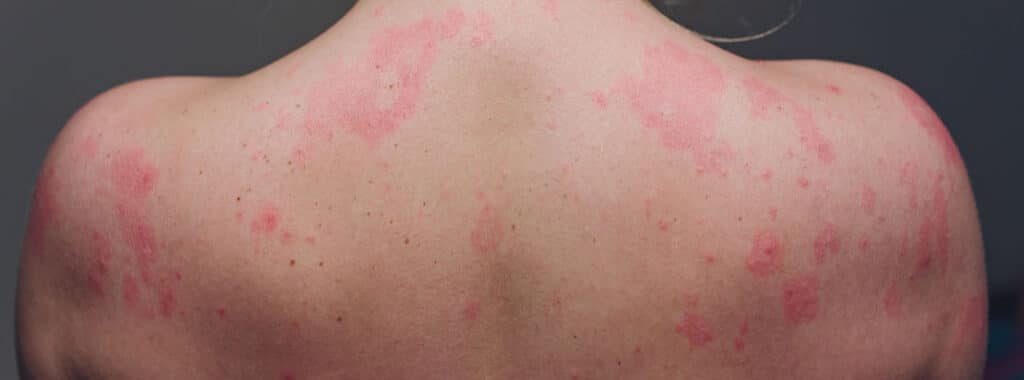
This is a medical term used to describe a change in the colour, texture or appearance of the skin. A rash can also be associated with other features such as itching and other symptoms, e.g. fever and chills. Rashes can be caused by many different things, so it is important to investigate the cause. Treatments may include moisturisers, creams, baths, cortisone creams that relieve swelling, and antihistamines, which relieve itching.
Rosacea is a common and debilitating issue of adults. There are a host of underlying contributing factors, including genetic factors, exposure to UV light, poor quality skin care, drying soap use, heat, alcohol and sometimes steroid creams.
It is characterised by central facial redness, small and superficial dilated blood vessels on facial skin, papules, pustules, and swelling. There can also be an associated grittiness of the eyes and also facial flushing. It most often affects those between 30-60 years of age. In severe cases, the eyes may be involved and nose can develop permanent lumpiness (“rhinophyma”).
Treatment is complex and can involve a combination a suitable set of skin care regime, creams, oral antibiotics or Vitamin A tablet (isotretinoin) and possibly laser treatments. Many patients are able to keep the symptoms under control with good, tailored skin care and dermatologist-prescribed medication. Our cosmetics nurse Kristie will also be able to assist you in choosing appropriate skin care and discuss options including laser.
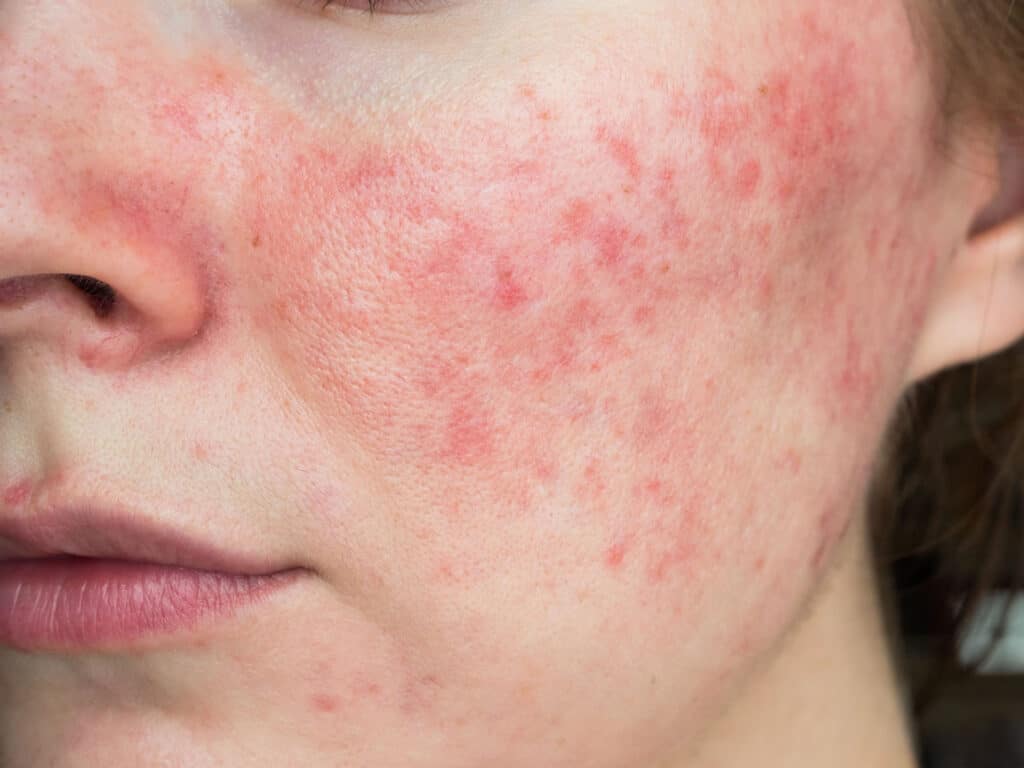
Skin allergy or contact dermatitis is quite common. This is a hypersensitive reaction by the immune system to a substance, food, object or chemical, which causes a skin rash and other symptoms.
As dermatologists, we do see allergic contact dermatitis, which is where there is a reaction on the skin to a compound you may be allergic to. The common culprits that we see at our clinic in South Melbourne include cosmetic products, baby wipes, hair dyes, perfumes, cosmetics and household products such as rubber/leather gloves, glues, paints and sprays.
To investigate allergic contact dermatitis, we work closely with immunologists/allergists to determine any potential allergies. Our experienced dermatologists may want to send you for patch testing which may be able to pin-point the exact allergens that you need to avoid.
If you have a persistent skin rash and you suspect allergy, please come for a full assessment by our Dermatology team. Dr Hope Dinh also works alongside the Patch Testing Team at the Alfred Hospital in the outpatients clinic.
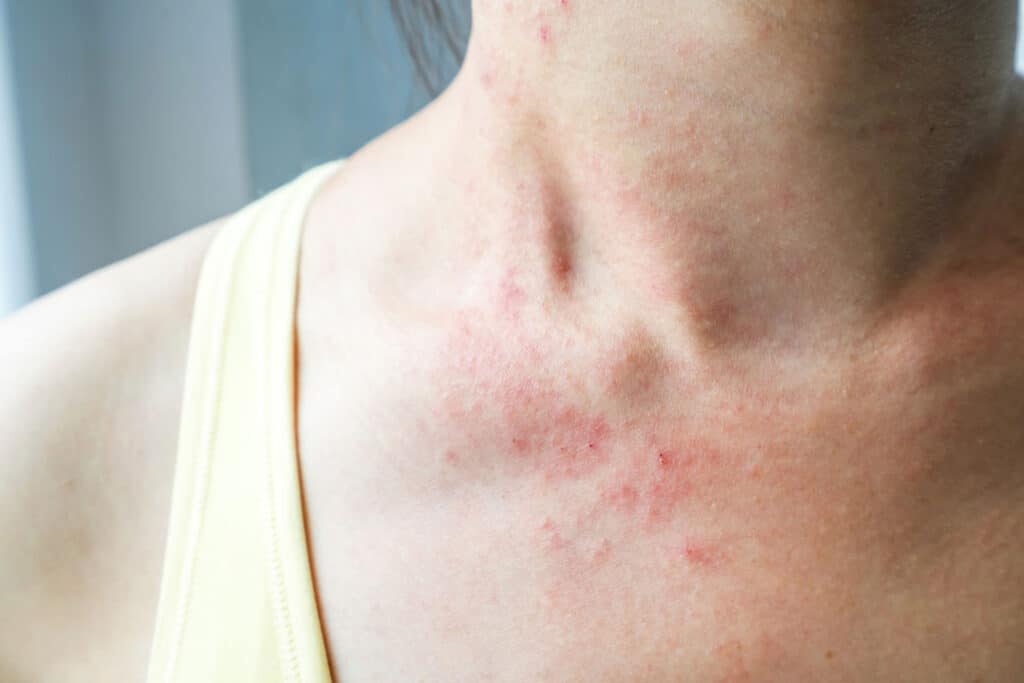
Hives, otherwise called urticaria, is an outbreak of swollen, itchy pale red bumps or plaques on the skin that appear suddenly and usually self resolves within a few hours to days. The lesions migrate around the body. The best course of action is to avoid the trigger if it is known. Antihistamines can assist and there are a number of other medications for chronic urticaria.
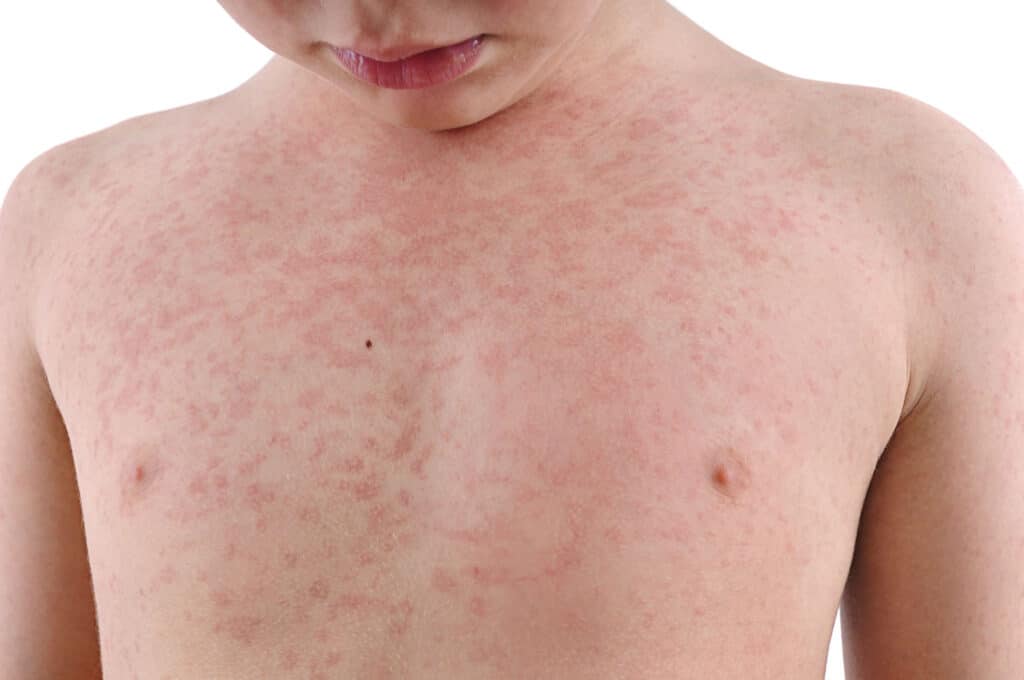
Vitiligo refers to depigmented skin where the cells producing our skin colour have been attacked by the body’s own immune system. Vitiligo can affect all ages; from children to adults. Vitiligo can occur with other autoimmune conditions such as thyroid disease, pernicious anaemia or diabetes.
The pale, depigmented areas are prone of burning with sun exposure. There are various sub-types of vitiligo including localised, generalised and segmental. Treatment depends on the location of the vitiligo and how extensive the condition is.
Treatments include creams, injections, UV phototherapy or Excimer laser treatments. Exciting new developments in vitiligo include pigment cell grafting but this is reserved for more severe cases. Our team of expert dermatologists have many years of experience in treating vitiligo and understand its cosmetic impact. We welcome new referrals.
