Category Archives: Uncategorized
Rough, red and raised bumps? This could be keratosis pilaris!
This could be keratosis pilaris (KP). This is a harmless and manageable skin condition. Although...
Jun
Help me with my acne in pregnancy!
Acne During Pregnancy: How to Manage It Safely and Effectively Acne during pregnancy can be...
Mar
ECZEMA? RED, SORE, ITCHY, DRY SKIN……LETS GET RID OF IT! 😊
Atopic Dermatitis is a skin condition that usually develops in early childhood and is more...
Jan
UVB Phototherapy
What is UVB Phototherapy? It is treatment with shortwave ultraviolet radiation. Here at Hope Dermatology,...
Jul
Skin Cancers – What you need to know
Confused as to what skin cancers are? Which are the most dangerous? How are they...
Nov
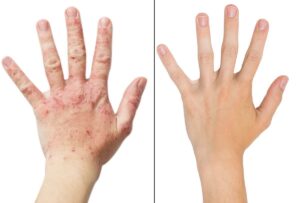
Hand Dermatitis in COVID-19 times
In this stressful time of COVID-19, all of us are doing the right thing and...
May
Alopecia Areata
Have you noticed bald patches appearing on your scalp or just general thinning of the...
Nov
Say Goodbye To Hyperhidrosis (Excessive Sweating)
Do you suffer from excessive sweating, have to change your shirts multiple times a day...
Oct
Biologics?! Hives? Psoriasis? Hidradenitis Suppurativa? There is an effective treatment!
Have you been suffering with the chronic itching of hives or are areas of your...
Sep
What is molluscum contagiosum?
Molluscum Contagiosum You may have experienced a bumpy rash like condition but unsure what it...
Jul