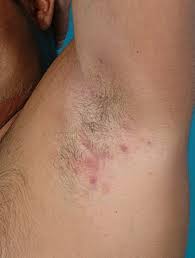
Hidradenitis Suppurativa (HS) – the latest information from the recent Melbourne Dermatology Conference May 2019.
Every year the Australasian College of Dermatologists holds an annual scientific meeting to update us all on the latest advancements in the diagnosis and management of dermatologic diseases. This year it was held in Melbourne (YES – my home town!). After 4 days of absorbing all this amazing information, my head is bursting with ideas for managing our existing patients. One session that really got my attention was the hidradenitis suppurativa lecture. Mainly under-diagnosed and sub-optimally managed, the prevalence of this condition is 0.67% (so, it’s more common than you think!). It was pleasing to hear that dermatologists lead the list of the medical specialists diagnosing this condition but there is STILL a LONG delay of MANY YEARS to patients being formally diagnosed with this condition.
WHY?
There can be many factors leading to diagnosis delay including embarrassment from the patient about the condition and so they never speak up about it, sub-optimal education of other medical specialties about the condition, patients thinking it is just a “simple boil” in the groin etc ……in order to diagnose HS earlier, the public needs to be more aware that a condition like HS even EXISTS…..
We really should be asking our patients – “Do you suffer from sore painful lumps or boils under your armpits or groin area?? Do you mind if I have a look? As it could be hidradenitis suppurativa.”
“SEEK and YOU WILL FIND”
_____________________________________________________________________________
Hidradenitis suppurativa is an inflammatory skin disease that affects gland-bearing skin in the underarms, in the groin, and under the breasts. It is characterised by recurrent boil-like nodules and abscesses that culminate in pus-like discharge, difficult-to-heal open wounds (sinuses) and scarring. Hidradenitis suppurativa also has significant psychological impact and many patients suffer from impairment of body image, depression and anxiety.
Hidradenitis often starts at puberty, it is most active between the ages of 20 and 40 years, and in women, can resolve at menopause. It is three times more common in females than in males. Risk factors include:
- Other family members with hidradenitis suppurativa
- Obesity and insulin resistance/metabolic syndrome
- Cigarette smoking
- Acne
- Inflammatory bowel disease
- Rare autoinflammatory syndromes
Signs and Symptoms
HS can affect single or multiple areas in the armpits, neck, sub mammary area, groin and inner thighs. Anogenital involvement most commonly affects the groin and vulva (in females), sides of the scrotum (in males), buttocks and perianal folds.
- Open and closed comedones (white heads and blackheads)
- Painful firm papules, larger nodules and pleated ridges
- Pustules, fluctuant pseudocysts and abscesses
- Draining sinuses (like “tunnels” under the skin) linking inflammatory lesions
- Thick (hypertrophic) scarring
Hidradenitis can be associated with inflammatory bowel disease and so it is important for your dermatologist to also consider screening for your risk of this condition too. HS can also be associated with acne, psoriasis and hirsutism.
General measures you can do at home
- Loose fitting clothing
- Avoiding too much friction in affected areas (being careful with the types of exercise pursued). It may be worth considering the High Intensity Workout regimes which get your blood pumping quickly but minimise too much frictional irritation.
- Reduction in weight (to lead to decreased friction in the skin fold areas); dietician advice may be helpful
- Daily un-fragranced antiperspirants
- If prone to secondary infection, wash with antiseptics or use dilute bleach baths
- Apply simple dressings to draining sinuses
- Analgesics, such as paracetamol (acetaminophen), for pain control
- Seek help to manage co-existing mood issues such as anxiety and depression
- Seek GP advice about weight loss, mood issues, quitting smoking etc. Also GPs can act and possibly come up with Team Care Arrangements which then allow patients to access some allied health services for FREE (like dietician consults and psychological support).
- Join a support group so you can receive tips and support from people who going through the EXACT same issues as you!
We are here to help you manage your disease!
The dermatologist may prescribe local therapies such as –
- anti-septic washes (such as Phisohex or Chlorhexidine),
- antibiotic cream (such as Clindamycin 1% cream),
- injections of steroid solution into the inflamed lumps.
- Topical vitamin A creams (retinoids) to help unblock the blackheads and whiteheads
Oral medications include –
- Oral contraceptive pill or hormonal treatments such as spironolactone (for females).
- Oral antibiotics to clear any infection and reduce inflammation (must be taken for a few months to see the outcome).
- Vitamin A tablets such as isotretinoin or acitretin
- Metformin (a diabetic medication) which can help with the insulin resistance pathway which can drive HS
- Oral immunosuppression tablets
Injectables
- There are the new injectable “biologic” medications which have recently been approved under the PBS for eligible patients with hidradenitis.
Surgery
- Simple surgery that can be done at the dermatologist without general anaesthetic. This is the technique of de-roofing the very inflamed lesions to allow for healing.
- More complex surgery can be done in hospital via Plastics and usually done with consultation with the Dermatology Team.
Key points to remember
– Get the correct diagnosis from a professional such as a dermatologist EARLY, don’t mistake it just as a pimple
– Early treatment can mean less chance of scarring
– There are simple home measures you can do to prevent them from flaring
– With appropriate treatment you can stop this disease from returning
Want to know more? Here are some online resources
https://www.dermnetnz.org/topics/hidradenitis-suppurativa/
http://anzvs.org/patient-information/hidradenitis-suppurativa/
http://hidradenitissuppurativasupportgroup.org/